There’s an astonishingly simple way to make PrEP available for all. What’s the government waiting for?

Matt Hancock, health secretary, leaves 10 Downing Street. (Chris J Ratcliffe/Getty Images)
Ian Green, chief executive of HIV charity Terrence Higgins Trust, writes for PinkNews how, with the money for PrEP secured, now is the time for the government to ensure the life-saving pill is available to all.
Today (1 April) marks a milestone in the course of the HIV epidemic in England.
A serious cash injection by the government now means more people should be able to access the HIV prevention drug PrEP.
But we need more than just money to unleash its true potential.
We must get it in the hands of more people who urgently need it, into the NHS service all communities use week-in, week-out. Otherwise, we risk letting down communities whose lives continue to be disproportionately impacted by HIV.
In my five years leading Terrence Higgins Trust, PrEP has been a constant issue we’ve been battling on.
Alongside other charities, activists, and clinicians we successfully lobbied for PrEP to be made available on the NHS.
This wasn’t easy but after a court battle led by our friends at National AIDS Trust, then a three-year capped trial, last March the health secretary Matt Hancock finally announced PrEP would be available free on the NHS via sexual health clinics.
The roll-out of PrEP hasn’t been as fast as we’d like to have seen but owing to the unprecedented pressures of COVID-19, it had to be done in a more piecemeal fashion.
Now as we begin coming out of lockdown 3.0, news of a significant uplift in funding for the delivery of PrEP over the next year ahead is welcome.
This £23 million is very timely – as restrictions ease, many people will start having sex, or more sex with more partners – again.
A doubling of PrEP funding must be followed by an expansion of services where PrEP is available. Making it routine in sexual health clinics has been a revolution for gay and bisexual men in urban areas but it fails too many.
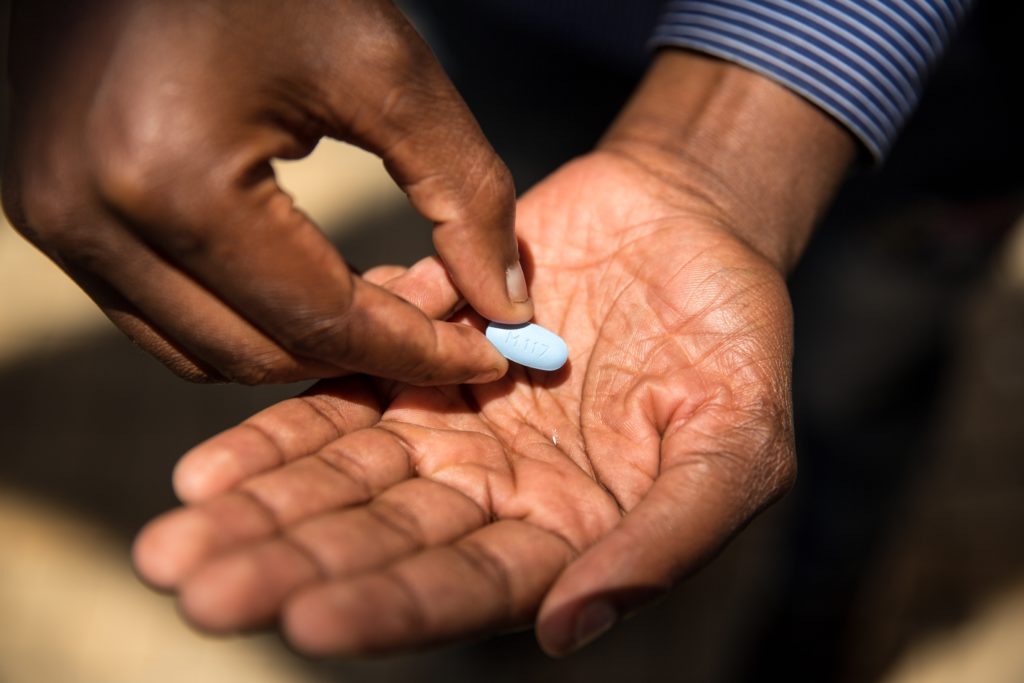
Pre-exposure prophylaxis, or known simply by ‘PrEP’, is a common antiviral drug. (Getty)
LGBT+ people in rural areas, women and men of Black African heritage, and many others are being left behind. PrEP, put simply, needs to be in the health services most used by people UK-wide: GP surgeries, community pharmacies, and other NHS services – A&E, termination clinics, and much more besides.
Women – who unbeknown to most make up one-third of people living with HIV and one-quarter of new HIV diagnoses in 2019 – are particularly hardest hit by this limited access point.
Women are much less likely to attend a sexual health clinic in the first place, those who do are twice as likely to decline an HIV test than men, with Black African women most likely not to be offered an HIV test and decline a test.
Meanwhile, trans people have told us they feel uncomfortable attending sexual health clinics due to misgendering, prejudice, and being given incorrect information for their bodies, with half saying they don’t feel in control of their sex lives.
PrEP empowers people to take charge of their sexual health in this regard.
The success of PrEP among gay and bisexual men has contributed to a 47 per cent drop in new cases of HIV among this population since 2014.
But we are not seeing that same progress happen in other groups impacted by HIV. Structural barriers, including racism and transphobia, are hampering efforts to increase the uptake of PrEP. This was reflected in the fact only four per cent of people on the NHS England PrEP trial were not gay and bisexual men.
Expanding PrEP access is a no-brainer.
But we already know where it would work. A report by the national HIV Commission last year identified GP surgeries, pharmacies, and gender identity clinics as some of the places where PrEP access could help normalise conversations about HIV and reduce new diagnoses.
To get this far has been a long and arduous battle – but this cannot be the limit of our ambitions. We need to take PrEP to the next level and dismantle all barriers to access.
We cannot do this on our own. I’m urging doctors, pharmacists, and nurses in the health service and director of Public Health, commissioners, and local councillors in health leadership roles to join us.
We have new money but do we have the political will across the country.
The government has already hinted it is looking at PrEP in other places as part of its up-and-coming new HIV Action Plan.
But delay is a disaster, means more will acquire HIV in the short term and the government’s own aim to end new cases of HIV by 2030 becomes more challenging by the day.
Matt Hancock should direct officials to start work on getting PrEP into the GP Core Contact and to create a new Patient Group Direction to allow pharmacists to dispense PrEP to their patients.
PrEP is now a reality and it’s long overdue that more people should be able to get their hands on this wonder drug.
It is important for those at risk of HIV and the only way we will make serious progress towards ending the domestic HIV epidemic.

