Media attacks just cost thousands of trans people failed by the NHS access to healthcare. But we will never desert those in need
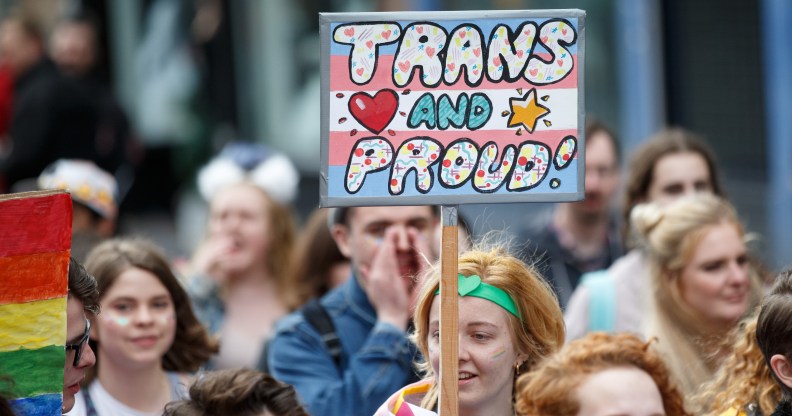
A participant holds a sign saying “Trans and Proud” during the Glasgow Pride. (Robert Perry/Getty Images)
After thousands of trans people lost access to their healthcare thanks to relentless anti-trans media coverage, Adi Daly-Gourdialsing, head of patient services at GenderGP, explains why the private clinic is unwavering in its commitment to providing healthcare for the trans community.
This week, the UK media reached a new low point as it once again attacked services providing support to trans youth.
Along with GenderGP (which is no stranger to the firing line), transgender youth charity Mermaids and trans-friendly pharmacy Clear Chemist came under attack.
Shockingly, Mermaids’ private forums were infiltrated, breaching the confidentiality of those who rely on this support group to help them through the challenges they face as parents of trans youth. Clear Chemist has been reported to its regulator, the General Pharmaceutical Council, and now feels limited in its ability to dispense to GenderGP patients for no other reason, it would seem, than the fact that they are transgender.
The media revealed (shock, horror) that waiting years for help leaves parents and their young people feeling abandoned by the NHS, that they are desperate for support and that in their desperation they turn to other parents for advice and guidance on how to navigate this incredibly stressful situation.
GenderGP was mentioned “more than 500 times” in the private forum as one way for parents to access the care they need, the media reported. This was a fact that the “investigative” journalist chose to hone in on as evidence of some wrongdoing. In reality, it is simply evidence of the fact that our service provides the much needed help that is so lacking and for which there is a desperate need.
What is GenderGP?
GenderGP is a private service providing affordable healthcare to transgender individuals. It does not discriminate on the basis of age, gender or geographical location. The inclusive service has been in operation since 2015, and during that time it has evolved from one GP answering a few emails into a fully fledged clinic supporting thousands of trans people around the world.
Not that it’s been an easy ride.
Despite facing hurdle after hurdle, including GMC investigations into not one but two incredibly committed doctors and a conviction for the service which subsequently had to move outside of the UK, the service has stayed strong and its commitment to the trans community has never wavered.
And why would it, when a very clear problem has been identified and a solution has been found?
In 2016, the Women and Equalities Commission bravely and unreservedly found that: “The NHS is failing in its legal duty under the Equality Act in this regard. There is a lack of continuing professional development (CPD) and training in this area amongst GPs. There is also a lack of clarity about referral pathways for Gender Identity Services. And the NHS as an employer and commissioner is failing to ensure zero tolerance of transphobic behaviour amongst staff and contractors.”
Fast forward to 2020 and little has changed. We still have: No NICE guidelines on the medical interventions available for gender incongruence; no standards of medical education set for this area of healthcare by the General Medical Council; no continuing professional development (this is the responsibility of the Royal Colleges and Postgraduate Deaneries); no agreed standards of care for NHS trusts and clinical commissioning groups; no UK-wide medical guidelines; and healthcare that is provided in super-specialised clinics, which are supposed to cater for just 500 patient cases per year.
If we cannot turn to private providers such as GenderGP, where does this leave trans healthcare?
With outdated protocol and practice that fills the social media forums with tales of suffering.
With extreme gate-keeping and care provided based on a postcode lottery system.
With protocols that are created and written by the consultants who are currently providing the failing care.
With specialist clinics that cannot possibly handle the numbers of patients requiring assistance.
With GPs and hospital consultants who are ‘allowed’ to deny care to trans patients. Afraid to help; safe if they avoid the subject altogether.
With arguments between the BMA, GMC, Royal Colleges as to whether GPs and hospital consultants should be forced to provide any level of care at all.
What is the solution?
There is urgent need for mandatory medical training and education. Not by the current specialists in the field, but by forward-thinking doctors who understand what it means to be trans, taking into account the views of service users, not the gender critics. Evidence-based, published guidance from centres of excellence needs to be adopted into UK protocol.
There need to be penalties for doctors who do not have the required level of basic skills and knowledge. Transgender care is not a specialist area of medicine – hormones are an area of medicine that every GP has a command of. Finally, and crucially, trans healthcare service options need to be brought into GP surgeries and local hospitals, so the healthcare is normalised, and trans people are no longer marginalised.
Accusations that there is no precedent, that there is no research, evidence or guidance available are simply untrue. Any healthcare professional looking to better understand this area of healthcare need only study research issued by more progressive countries to see the extent of the evidence that exists for the affirmative care of trans youth.
We need an amnesty for trans healthcare, a clean slate on which we can write a list of what great healthcare for this cohort would look like.
It’s not rocket science. This is what good trans healthcare looks like.
If you say you are trans, you will be believed.
You do not have to wear a dress to be accepted as a trans woman.
You do not have to have an overtly feminine or masculine name to be accepted as trans.
If you say you are trans then your mental health will not need to be evaluated.
You do not need to provide six months of assessments as “evidence” of your gender.
If a young person says they are trans, they will get the support they need to help them to come to terms with what that might mean.
You will not be forced to have therapy, but there will be plenty of support and education available for you and your loved ones, as needed.
If a young person needs to suspend puberty, to allay the terrific fear of those irreversible body changes and to give you all the chance to think clearly, that is completely understandable and totally doable.
If you want to try out gender-affirming hormones to see how they feel, you can. You will not turn into a “bearded giant” overnight nor will your breasts instantly appear.
If you want surgery, you can talk openly about it, how it is a big decision and what you are hoping it will achieve, and how you might feel if that isn’t achieved. And then you can work together with support to find a good surgeon, whose number one priority is your wellbeing.
If only there was a service that was already providing all of this to the trans community. A service that treated trans folk with dignity, respect and equality. A service that did its utmost to help trans people thrive, not just survive.
Oh wait, what was that service I heard about being referenced “more than 500” times on a Mermaids forum?
Adi Daly-Gourdialsing is head of patient services at GenderGP. Views expressed in this article are wholly hers and are not necessarily endorsed by PinkNews.

