NHS England urged to adopt full roll-out of HIV-preventing PrEP drugs

PrEP: Man holding a pill used for Pre-Exposure Prophylaxis (PrEP) to prevent HIV infection
NHS England has been urged to adopt a full roll-out of HIV-preventing drugs, rather than allow people to be turned away and left at risk of HIV.
Pre-Exposure Prophylaxis (PrEP) drug Truvada, which can drastically reduce people’s chances of being infected with HIV, was made available for free on the NHS last year as part of a large-scale three-year trial.
As part of the trial, 10,000 places were made available via participating sexual health clinics across England – with most of the places reserved for men who have sex with men.
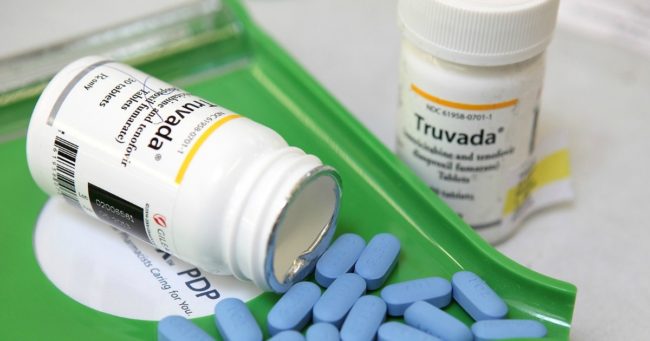
Pre-exposure prophylaxis (PrEP) drugs (Getty)
However, in several regions many of the major clinics involved in the trial were forced to close recruitment to gay and bisexual men, after their capacity for trial places was quickly filled due to high demand.
NHS England is considering adding another 3,000 places to the trial, but experts say the “stopgap” measure is not enough – and that many clinics will soon again be at capacity.
13 clinics are currently closed to recruitment for men who have sex with men due to capacity – ten of which are in London.
Today (July 17) a group of 32 charities and community groups, including Terrence Higgins Trust, National AIDS Trust, PrEPster and Stonewall have signed onto a joint statement warning that the trial capacity is not enough.
It says: “In June 2018 NHS England announced it is considering a proposal for a further 3,000 places to be made available on the trial.
“Whilst welcome, this provides only temporary relief. With continuing high demand for PrEP, clinics will again be full and turning people away within a few months. It is therefore not a sustainable solution.”
It added: “NHS England have committed to the provision of PrEP. With the trial only beginning in October 2017 and due to run for three years, we cannot wait until late 2020 to do something about the current situation.
“We need a national programme as soon as possible to ensure PrEP is made available to everyone in England who needs it.
“NHS England and local authority commissioners must start the process now to ensure PrEP is routinely available in sexual health clinics by 1 April 2019 at the latest.
“Both NHS England and local authority commissioners should agree and disseminate as soon as possible a timetabled roadmap of the necessary decision-making process.
“In the meantime a solution must be found to ensure no one in need of PrEP is turned away.”
Matthew Riley, 25, has been taking PrEP via NHS England’s IMPACT trial for six months.

Matthew Riley
He said: “I started PrEP after doing a lot of research. It gives me control over my sexual health and gets rid of the shadow that HIV, as a gay man, casts over my sex life. Being more comfortable with yourself and your health essentially means healthier, better sex.
“Financially, I wouldn’t have been able to buy PrEP for myself because I just don’t have the disposable income. Without the PrEP trial I wouldn’t have been able to access PrEP and it’s awful that other people, just like me, are being turned away.”
The letter is signed by National AIDS Trust, Terrence Higgins Trust, PrEPster, African Advocacy Foundation, Avert, BASHH, BHA, BHIVA, CAPS (Catholics for AIDS Prevention and Support), Clinic Q, Eddystone Trust, George House Trust, GMFA HERO, i-Base, iwantprepnow, Kernow Positive Support, LGBT Foundation, London Friend, Metro, NAM, Naz, NHIVNA, Positive East, Reshape, River House, Sophia Forum, Spectra, Stonewall, Trade, UK-CAB, Yorkshire Mesmac and Brigstowe
Yusef Azad, director of strategy at the National AIDS Trust, said: “Some people attempting to access the trial have been turned away from clinics with no places left, and gone on to acquire HIV. Those people will now be on medication for life when they could have been given a cost-effective prevention pill for shorter-term risk.
“There is no good reason to delay routine commissioning of PrEP so it can be accessed by all who need it.”
Ian Green, chief executive at Terrence Higgins Trust, said: “We have been clear that a 10,000 place trial was never going to accurately meet demand for PrEP – a highly effective way of preventing HIV. We know that some trial sites are full, some are yet to open and that eligible people are now being turned away.
“There is a clear moral, political and economic rationale for providing PrEP on our NHS to those who need it and that’s why a routine programme for PrEP on the NHS must happen as a matter of urgency.”
Will Nutland, co-founder of PrEPster, said: “With almost three-quarters of trial places taken, it is imperative that we now have a road-map for implementation of routine commissioning of PrEP.
“We know that PrEP works: now’s the time to make sure it’s available for everyone who needs it.”

