Australia may be about to publicly fund PrEP

PrEP
A leading health body in Australia has recommended that the health service in the country should publicly fund HIV-prevention drug PrEP (Pre-exposure Prophylaxis).
The Pharmaceutical Benefits Advisory Committee (PBAC) said that it will recommend the Pharmaceutical Benefits Scheme (PBS) subsidises the pill.
HIV testing kits are available at doctors surgeries (Photo by: BSIP/UIG via Getty Images)
The decision to recommend the prevention medication came after the body found it to be cost-effective and powerful in reducing HIV transmission.
PrEP was approved for use in the country last year by the Therapeutic Good Administration (TGA), however, a monthly prescription set users back by AUS$5000 a year, or $416 a month.
Once the medication becomes subsidised by PBS, it will cost just $39 for a prescription which is usually around 90 pills – or three months – worth of medication.
Concession cardholders will be able to obtain the medicine for just $6.30 for a prescription.
The decision has been welcomed by LGBTQ and HIV/AIDS activists in the country who have called it a “critical” step to reducing HIV transmission.
Darryl O’Donnell, the chief executive of the Australian Federation of AIDS Organisations (AFAO) said that despite it being a step in the right direction, a “great effort to promote awareness was still needed.
O’Donnell said: “Gay and bisexual men continue to carry the greatest burden of HIV in Australia, and we expect that PrEP will sharply drive down rates of HIV for this community.
“But great effort will be needed to ensure PrEP access and awareness across all parts of the gay community.
“Additionally, Aboriginal and Torres Strait Islander people, migrant communities, and some heterosexual populations have seen starkly higher rates of HIV transmission over the last five years. While a PBS listing of PrEP is critical, we must make sure everyone who needs PrEP is aware of it and can access it.”
Related: What is PrEP and how can I get it? Everything you need to know about HIV-preventing drugs
President of the AIDS Council of New South Wales (ACON), Justin Koonin, added that the slab in the price for PrEP will hugely benefit more marginalised communities.
“There are three new HIV diagnoses each day in Australia and we expect the government will now move quickly to list PrEP on the PBS.
“Prevention of HIV is much cheaper than a lifetime of treatment and it makes good sense to have this medicine available to all who need it,” Koonin said.
Some people have raised concerns over the PBS’s ability to roll the medication out in a timely manner.
Chief Executive of the Victorian AIDS Council (VAC), Simon Ruth, explained: “There are 8,000 people in the NSW [PrEP] trial and 4,000 in the Victorian trial, so there are at least two thousand guys in Melbourne wanting to access PrEP – in the event of it being subsidised, there will be a lot of people seeking GP appointments very quickly.”

PrEP
Related: What is bareback sex and what do I need to know about it?
The decision to recommend PrEP be subsidised comes after neighbouring country New Zealand announced that it would be publicly funding it from March 1.
The country is one of a few that have made the decision to make the HIV prevention medication available at a reduced price of US$1.20 a month for a prescription.
Previously, a prescription for the drug would cost US$731 a month, meaning that many users would import the medication. Getting it from overseas would still cost around US$36 a month.
By publicly funding Truvada, the cost of a quarterly prescription will fall to just US$3.60, which works out to $1.20 a month making it cheaper than in almost any other country in the world.
PrEP is up to 99% effective at preventing HIV transmission.
Other countries to subsidize PrEP are Brazil, France, Norway, Brazil, Belgium and Scotland.
The World Health Organisation strongly backed the use of PrEP as HIV prevention in 2014, but global provision remains patchy.
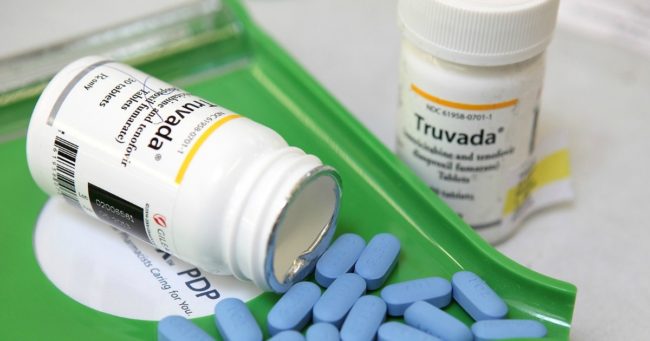
Pre-exposure prophylaxis (or PrEP)
Related: A once-a-week HIV pill could soon be available
In England, PrEP is now available on the NHS to at-risk groups including gay men for free as part of a three-year trial.
NHS England is investing £10 million in the trial. Privately, generic PrEP drugs are available for around £39 a month.
The cost of a public PrEP scheme is currently higher than buying the drugs privately, as Gilead still holds patents covering the provision. Branded Truvada costs £350 a month, and the cost of public PrEP schemes are projected to plummet once Gilead’s patents expire.
HIV researchers believe rolling out PrEP might actually be cost-effective in the long term.
As the lifetime cost of treating just one HIV infection can be up to £380,000, a PrEP scheme would only need to prevent a handful of transmissions in order to be cost-effective.

